DOCTOR INFORMATION
Uveitis
Uveitis is the third leading cause of blindness in developing countries. This is because patients are left on chronic steroid treatment leading to various complications like optic nerve damage, complicated cataract, glaucoma and many more. In this post we will explore what uveitis is, how can we diagnose different types of uveitis, and the treatment approach based on clinical signs, symptoms and types.
Contents:
 What is uveitis❓
What is uveitis❓
 Types and classification 🏨
Types and classification 🏨
 Anterior uveitis (causes, symptoms and treatment)
Anterior uveitis (causes, symptoms and treatment)
 Intermediate uveitis (causes, symptoms and treatment)
Intermediate uveitis (causes, symptoms and treatment)
 Posterior uveitis (causes, symptoms and treatment)
Posterior uveitis (causes, symptoms and treatment)
What is uveitis❓
 It is an inflammation of the uvea (the middle layer of eye between the retina and sclera) 👁
It is an inflammation of the uvea (the middle layer of eye between the retina and sclera) 👁
 The uvea is made up of the iris, the ciliary body (pars plicata and pars plana) and the choroid 👁
The uvea is made up of the iris, the ciliary body (pars plicata and pars plana) and the choroid 👁
 Inflammation of these structures is called:
Inflammation of these structures is called:
- Iris: iridacycitis or iritis
- Choroid: choroiditis
- Ciliary body: cyclists or pars planitis for pars plana, and pars plicatis for pars plicita
 In some cases this inflammation can also affect affect the lens, retina, optic nerve and vitreous 👁
In some cases this inflammation can also affect affect the lens, retina, optic nerve and vitreous 👁
Summary:
Uveitis is the inflammation of the uvea. The uvea is the middle layer of the eye, between the retina and sclera.
Classification of uveitis
Based on anatomy:
1. Anterior uveitis:
 Iris and pars plicata are affected 👁
Iris and pars plicata are affected 👁
 Iris is close to the pars plycata of the ciliary body, and so, when the iris is affected, the pars plycata is usually affected too
Iris is close to the pars plycata of the ciliary body, and so, when the iris is affected, the pars plycata is usually affected too
 It is also called iridocylitis
It is also called iridocylitis
 It is the most common type of uveitis❗
It is the most common type of uveitis❗
2. Intermediate uveitis:
 Pars plana and vitreous are affected 👁
Pars plana and vitreous are affected 👁
 Pars plana is close to the vitreous, and so, when the pars plana is affected, the vitreous is usually affected too
Pars plana is close to the vitreous, and so, when the pars plana is affected, the vitreous is usually affected too
 It is also called vitritis
It is also called vitritis
3. Posterior uveitis (choroid):
 The choroid is affected
The choroid is affected
 It is also called choroditis
It is also called choroditis
4. Pan uveitis:
 All the parts of the uvea are affected 👁
All the parts of the uvea are affected 👁
 It is the most serious condition 🏨
It is the most serious condition 🏨
 Luckily, it is rare❗
Luckily, it is rare❗
 It is usually seen in sympathetic opthalmitis and Vogt Koyanagi Harada syndrome
It is usually seen in sympathetic opthalmitis and Vogt Koyanagi Harada syndrome
Acute and chronic classification:
1. Acute:
 Very common in primary stages, or uveitis which is present for less than 3 months 📅
Very common in primary stages, or uveitis which is present for less than 3 months 📅
2. Chronic:
 Any uveitis present for more than 3 months is considered chronic uveitis 📅
Any uveitis present for more than 3 months is considered chronic uveitis 📅
Granulomatons and Non-Granulomatons classification
1. Granulomatons:
 Uveitis caused by diseases which form granuloma 🏨
Uveitis caused by diseases which form granuloma 🏨
 E.g. TB, leprosy, scarcodosis
E.g. TB, leprosy, scarcodosis
 It is not very common❗
It is not very common❗
2. Non granulomatons:
 Uveitis caused by diseases which do not form granuloma 🏨
Uveitis caused by diseases which do not form granuloma 🏨
 It is a common condition❗
It is a common condition❗
Writing a diagnosis for uveitis
 Note that when writing a uveitis diagnosis, we need to mention all three classifications ❗
Note that when writing a uveitis diagnosis, we need to mention all three classifications ❗
 E.g. acute, anterior, non-granulomatos uveitis
E.g. acute, anterior, non-granulomatos uveitis
Summary:
Uveitis can be classified based on: anatomy (anterior, intermediate, posterior or pan), acute or chronic, and granulomatous or non-granulomatons. When diagnosing uveitis, you should refer to all 3 of these classifications.

Anterior Uveitis
 It is very common, almost 70% of all uveitis cases are anterior uveitis❗
It is very common, almost 70% of all uveitis cases are anterior uveitis❗
Causes:
 The most common cause is idiopathic 🏨
The most common cause is idiopathic 🏨
 HLAB-27 spondaloarthropathies (it is a group of 4 diseases: Alkylosing spondylitis, IBD inflammatory bowl disease, psoriatic arthritis, Reiter’s syndrome [reactive arthritis])
HLAB-27 spondaloarthropathies (it is a group of 4 diseases: Alkylosing spondylitis, IBD inflammatory bowl disease, psoriatic arthritis, Reiter’s syndrome [reactive arthritis])
 Juvenile arthritis (JRA)
Juvenile arthritis (JRA)
Presentation:
 Recurrent presentation of uveitis 🔄
Recurrent presentation of uveitis 🔄
Symptoms:
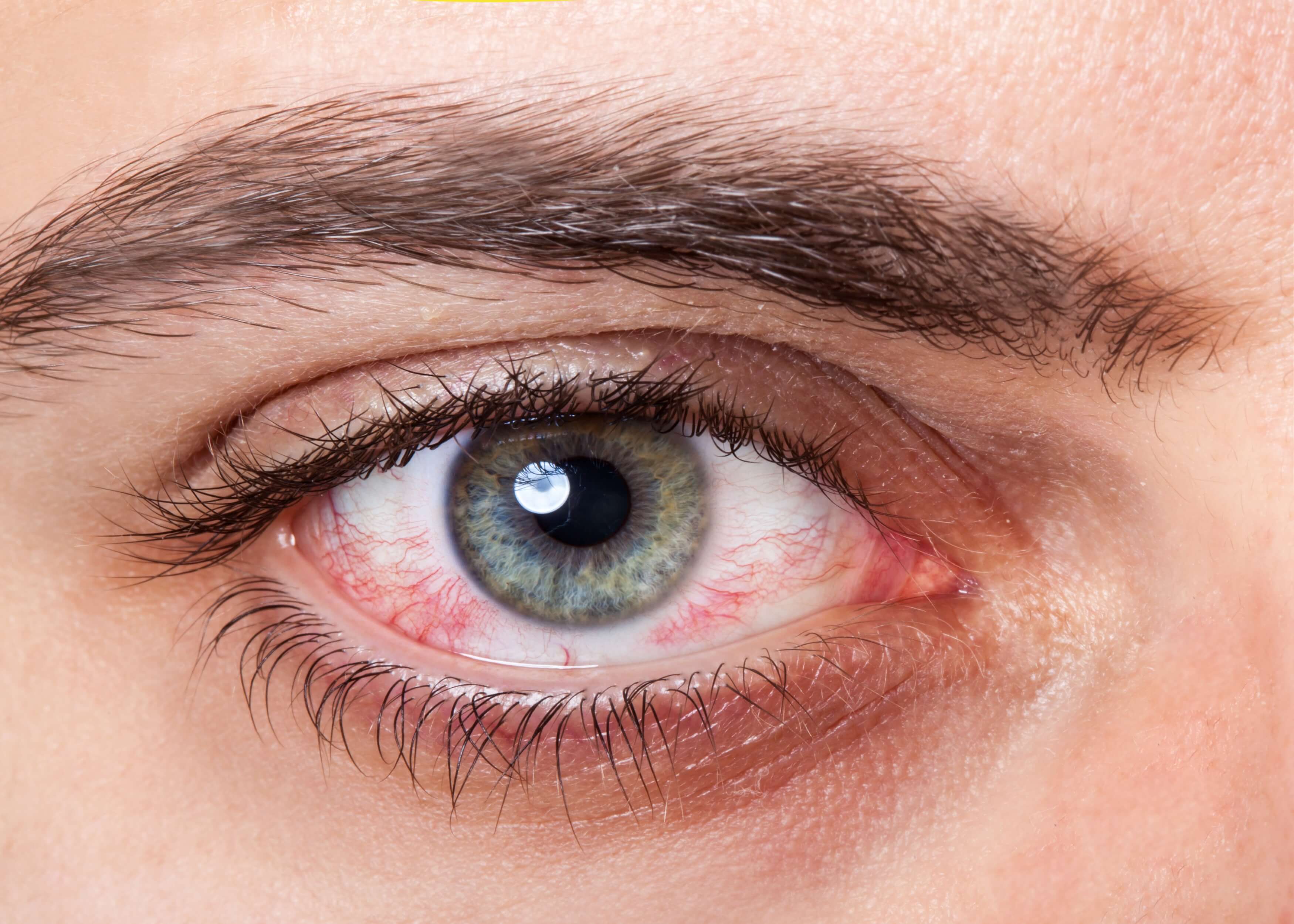
 Sudden red eye with pain and loss of vision 😖
Sudden red eye with pain and loss of vision 😖
Signs:
1. Circumciliary congestion 👁
 Bluish red
Bluish red
 Radical cell
Radical cell
 Wbc and neutrophils present in anterior chamber
Wbc and neutrophils present in anterior chamber
 Identified by slit lamp examination
Identified by slit lamp examination
 It is the earliest sign
It is the earliest sign
2. Flare 👁
 Protein deposits is seen in aqueous humor
Protein deposits is seen in aqueous humor
 This flare is the result of inflamed blood vessels due to this inflammation. Serum protein leaks out and mixes with aqueous humor causing aqueous humor, which is clear in normal conditions, becomes cloudy, opaque, or thick due to the serum protein which splits light
This flare is the result of inflamed blood vessels due to this inflammation. Serum protein leaks out and mixes with aqueous humor causing aqueous humor, which is clear in normal conditions, becomes cloudy, opaque, or thick due to the serum protein which splits light
 This is called flare
This is called flare
3. Keratic precipitates (kp) 👁
 Here we can see neutrophils and lymphocytes on the cornea
Here we can see neutrophils and lymphocytes on the cornea
 Flare, keratic precipitate, iris nodules, synechiae, meiosis, hypopyon
Flare, keratic precipitate, iris nodules, synechiae, meiosis, hypopyon
Complications of anterior uveitis:
 Glaucoma and cataracts
Glaucoma and cataracts
Treatment of anterior uveitis:
 Topical steroids: as inflammation is on anterior part (drug of choice) 💊
Topical steroids: as inflammation is on anterior part (drug of choice) 💊
 Cycloplegics: it paralysis ciliary muscle 💊
Cycloplegics: it paralysis ciliary muscle 💊
 Atropine, homotropine, cyclopantolate, tropicamide 💊
Atropine, homotropine, cyclopantolate, tropicamide 💊
Summary:
Almost 70% of all uveitis cases are anterior uveitis. The most common cause is idiopathic, and its presentation is recurrent with symptoms of sudden red eye with pain and loss of vision. Signs include: circumciliary congestion, flare, keratin precipitates. Complications include: glaucoma and cataracts. Treatment includes: topical steroids, cycloplegics, atropine, homotropin, cyclopantolate, tropicamide.
Intermediate uveitis
 This is the inflammation of pars plana and vitreous 🏨
This is the inflammation of pars plana and vitreous 🏨
 It occurs mostly in young people and children
It occurs mostly in young people and children
 It is not very common
It is not very common
Causes:
 Most common is idiopathic 👁
Most common is idiopathic 👁
 Sarcoidosis
Sarcoidosis
 Multiple sclerosis
Multiple sclerosis
 Cystoid macular edema
Cystoid macular edema
Symptoms:
 No redness, no pain, rare loss of vision ❌
No redness, no pain, rare loss of vision ❌
Signs:
 Floaters or muscae, snow balls or snow banks (if more snow balls are accumulated)
Floaters or muscae, snow balls or snow banks (if more snow balls are accumulated)
Treatment:
 Injectable steroid like triamcinolone (sub tenen’s injections is given due to the distance of intermediate uveitis)
Injectable steroid like triamcinolone (sub tenen’s injections is given due to the distance of intermediate uveitis)
 Subteaneals is better but more dangerous as it is close to the sclera, meaning it could perforate the sclera 😖
Subteaneals is better but more dangerous as it is close to the sclera, meaning it could perforate the sclera 😖
Summary:
This is the inflammation of pars plana and vitreous. Idiopathic causes are most common and it usually occurs in young people/children.There is no redness or pain and rarely, loss of vision. Treatment: injectable steroids.
Posterior uveitis
 This is inflammation in the choroid (also called choroiditis) 🏨
This is inflammation in the choroid (also called choroiditis) 🏨
Causes:
 Due to infection like toxoplasmosis, toxocariasis, cyclomagalo virus, HIV, herpes, TB
Due to infection like toxoplasmosis, toxocariasis, cyclomagalo virus, HIV, herpes, TB
 Small group of immune disorders like scarcoidosis, polyardisnodosa(PAN), scleroderma
Small group of immune disorders like scarcoidosis, polyardisnodosa(PAN), scleroderma
Symptoms:
 No pain
No pain
 No redness
No redness
 Loss of vision as the choroid is close to retina (even the retina gets inflamed due to the choroid inflammation, and so, in clinical practice we mostly see chorioretinitis) ❌
Loss of vision as the choroid is close to retina (even the retina gets inflamed due to the choroid inflammation, and so, in clinical practice we mostly see chorioretinitis) ❌
 Retina blood vessels also get inflamed (also called vasculitis) 👁
Retina blood vessels also get inflamed (also called vasculitis) 👁
 The vitreous sometimes gets inflamed too (called vitrities) in very severe cases
The vitreous sometimes gets inflamed too (called vitrities) in very severe cases
 You can find a combination of any of these three conditions, however, chorioretinitis is most commonly seen 👁
You can find a combination of any of these three conditions, however, chorioretinitis is most commonly seen 👁
 People usually visit the doctor when they experience loss of vision
People usually visit the doctor when they experience loss of vision
 On examination, if you see a yellow creamy patch below the blood vessels of retina then it is inflammation of choroid
On examination, if you see a yellow creamy patch below the blood vessels of retina then it is inflammation of choroid
Summary:
This is inflammation in the choroid. It is most commonly caused by infection. There are no symptoms of pain, redness but there is loss of vision, inflammation of retina blood vessels and the vitreous.
Summary:
- Uveitis is the inflammation of the uvea
- Uveitis can be classified based on: anatomy (anterior, intermediate, posterior or pan), acute or chronic, and granulomatous or non-granulomatons
- Almost 70% of all uveitis cases are anterior uveitis
By Megha Mehta













